Aging is a process of systemic degeneration involving a variety of tissues and organs in the whole body and is characterized by gradual reduction of regenerative ability and functional decline. In trying to understand the aging process, and more importantly, in pursuit to reverse it, scientists have developed a technique called heterochronic parabiosis (HP), which surgically connects the circulatory systems of a young and old animal, thus providing a unique paradigm for evaluating how tissues and organs respond to the opposite milieu at a systemic level.
Using HP, the revitalizing power of young blood was demonstrated in the late 1950s and early 1960s. Since the early 2000s, interest in HP has revived. Despite this renewed interest, though, how young blood makes aged bodies return to a “younger state” has so far remained a mystery.
In a recent study published in Cell Stem Cell, researchers from the Institute of Zoology and the Beijing Institute of Genomics of the Chinese Academy of Sciences probed the effects of HP in mice at the single-cell level, generating a systemic atlas of HP and aging.
With this atlas in hand and followed by functional validations, the researchers revealed cellular and molecular changes in the aged and young parabionts at single-cell resolution. More importantly, they revealed key mediators of the systemic effect and their cellular targets. This information may eventually provide important clues for the development of aging biomarkers in humans as well as new therapeutics for aging intervention.
According to the researchers, exposure to old blood can accelerate aging of various organs/tissues and cell types in the young parabiont, while reciprocally, exposure to young blood can elicit rejuvenation in the aged parabiont, especially through targeting the stem/progenitor cells and their niches in aged tissues across systems.
Adult stem cells continuously self-renew to maintain the somatic cell population and repair age-related damage. These activities are actively supported by neighboring or niche cells, and instructed by systemic factors that elicit intrinsic alterations directly in the stem cells or the niche environment.
The researchers determined that the activated stem/progenitor cell population includes basal stem cells and hair follicle stem cells (HFSCs) in skin; fibroblast/adipose progenitor cells (FAPs) in skeletal muscle; and hematopoietic stem and progenitor cells (HSPCs) located in bone marrow.
Aged HSPCs are among the cells most sensitive to young blood, whose exposure switches the transcription regulation network of HSPCs to a younger state, thus regaining the potential for lymphoid differentiation and restoring the population of lymphoid cells (such as pro-B cells) in aged bone marrow.
Notably, using a sophisticated CD45 congenic system to trace cell origins in parabionts, researchers verified that the rejuvenation effects were due to activation of aged HSPCs rather than relocation of young HSPCs from the other parabiont into the bone marrow. This discovery has clarified a puzzling issue by demonstrating a certain degree of cellular compartmentalization despite a conjoined circulatory system.
Moreover, the researchers identified a series of HSPC aging regulators including epigenetic regulatory factors such as YY1 and chemokines such as CCL3. For validation, researchers used mouse transplantation experiments to show that lentivirus-mediated YY1 overexpression could effectively enhance the reconstructive ability of aged HSPCs while similar “gene therapy” based on CCL3 overexpression could significantly improve the ability of aged HSPCs to differentiate into lymphoid cells.
In addition, several candidate targets, especially in pathways that reduce inflammation and restore cellular communication, were also identified, thus providing new rejuvenation strategies for solid tissues.
All in all, this multi-organ, multi-dimensional study reveals various key factors regulating the "rejuvenation" of adult stem cells and surrounding somatic cells, providing rich data resources for the establishment of new biomarkers and intervention strategies for aging. This work thus provides a new paradigm for discovering the “youth factors” from the perspective of systems biology.
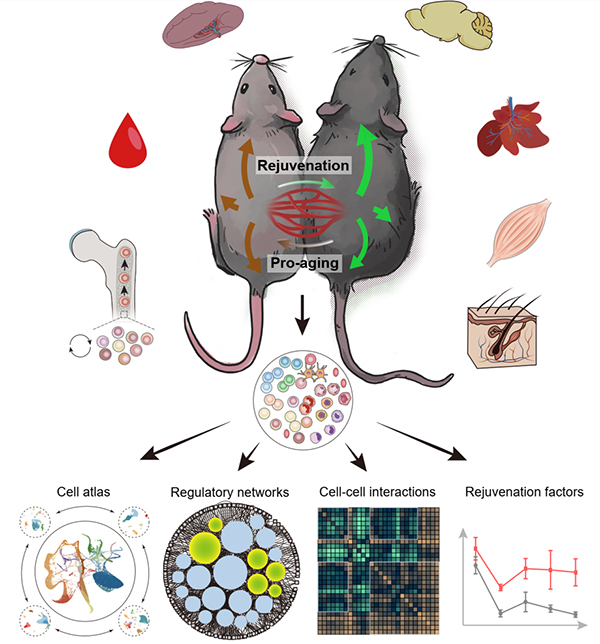
Figure 1. Systematic biology study on how young blood promote the rejuvenation of multiple tissues and organs (Image from Ma et al. Cell Stem Cell 2022)
Original link: https://doi.org/10.1016/j.stem.2022.04.017
Contact:
Guang-Hui Liu
Institute of Zoology Chinese Academy of Sciences
Tel: 86-64807852
E-mail: ghliu@ioz.ac.cn
Web: http://english.ioz.cas.cn/

